 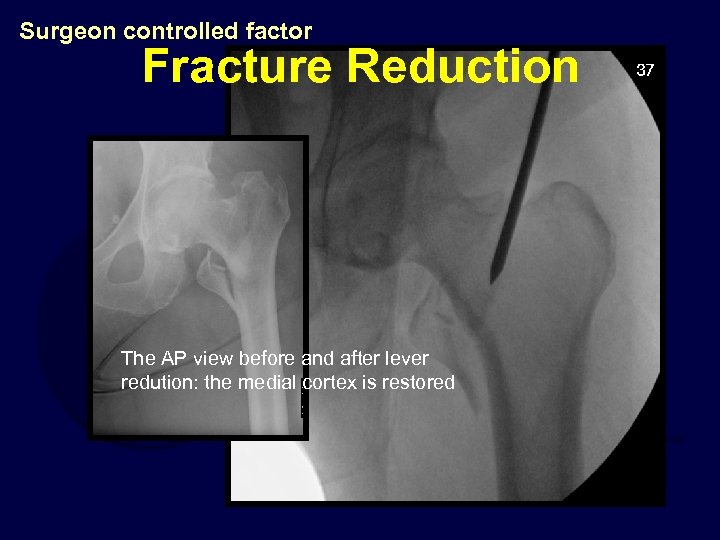
Besides, other complications including femoral neck shortening (FNS) and loss of neck‐shaft angle (NSA), although less emphasized by the literature, are virtually more common It is reported that the incidence of postoperative varus collapse with the cutout was between 1.5% and 6.5% With the increasing use of the CMN, associated failures have been continuously reported in the past decades, which typically presented as nonunion or malunion of the fractures with lag screw/blade cutout or cut‐through Thus, current guidelines and consensus support that, in managing unstable intertrochanteric fractures, CMN is preferable to the extramedullary devices Studies about implant loading confirm that the load to an implant is increased with varus mal‐reduction or with decreasing stability of the fracture, and that in these cases the intramedullary device can bear greater load than the extramedullary device In the past decade, cephalomedullary nail (CMN) has gradually become the most frequently used implant to intertrochanteric fractures due to its biomechanical advantages A report from Evidence‐Based Working Group in Trauma analyzed all the evidence and concluded that failure rates of treatment of unstable trochanteric fractures with a DHS are too high to recommend its use However, there are consistent concerns about the high failure rate associated with the use of the DHS in an unstable situation DHS has been shown to be the most cost‐effective option and has produced consistently good results in treating stable fractures. According to the AO/OTA Classification of Fractures and Dislocations, there is currently little evidence of the superiority of one device over another when the intertrochanteric fracture is stable (type A1 to A2.1) The recent consensus is that the implant options for the treatment of intertrochanteric fractures are closely related to the stability of the fractures There is literature about comparisons between these implants, including biomechanical characteristics, indications, complications, and outcomes Dynamic hip screw (DHS) as an extramedullary construct or intramedullary nail with a cephalomedullary screw is the standard surgical treatment option chosen by most surgeons. Achieving stable reduction and rigid fixation of the fracture and permitting immediate mobilization are the keys to this end The goal of care is to restore limb function with the lowest possible rate of surgical and medical complications. 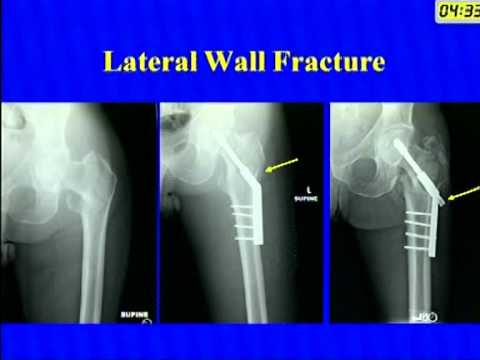
In patients over 50 years of age, more than 90% of hip fractures are intertrochanteric fractures with 20%–30% of these cases experiencing complications and a mortality rate of approximately 17%Īs there is high morbidity and mortality associated with historical nonoperative treatment, surgical management with internal fixation is commonly necessary for these fractures. Approximately half of all hip fractures are intertrochanteric femoral fractures, defined as extracapsular fractures that occur between the greater and lesser trochanter of the proximal femur These fractures are responsible for the largest use of resources for orthopaedics trauma around the world According to the epidemiologic projections, the worldwide annual number of hip fractures is estimated to rise from 1.66 mn in 1990 to 6.26 mn by the year 2050 With the rising life expectancy of the global population, the number of elderly individuals is increasing in every geographical region. These fractures have been recognized as the most serious consequence of osteoporosis because of its complications, which include disability, chronic pain, diminished quality of life, and premature death. Hip fractures are prevelant in the elderly population and are commonly caused by a low‐energy injury mechanism such as a fall from standing height. The purposes of the study are as follows: (i) to evaluate the efficiency of the current established CMN techniques (ii) to quantify the loss of reduction under an appropriately implanted CMN to anatomically realigned intertrochanteric fractures and (iii) to explore the possible underlying causes for the inevitable loss of reduction. However, until now there has been no research to explore whether the reduction loss after the operation can be fully prevented in the best cases. Many attributed this complication to misoperation during the surgery and hold that a series of techniques and tips could help to avoid the loss of reduction. However, a degree of reduction loss during bone healing is still not rare in clinical work. The implant design and fixation techniques of the cephalomedullary nail have been continuously improved to ensure uncomplicated bone union during the past decade. At present, cephalomedullary nail is the most frequently used implant in the management of intertrochanteric fractures around the world. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
